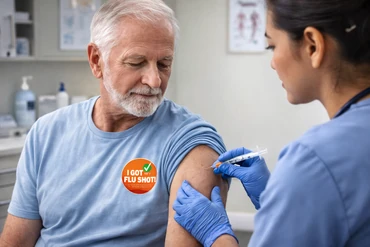
A new study conducted by researchers from Johns Hopkins University revealed that the body’s immune response to vaccines could become compromised as consumers age.
The researchers framed the study in the context of women, who were found to respond better than men to the flu vaccine. However, those stats declined as women aged into menopause, prompting the researchers to rethink the specifics when it comes to giving vaccines to older people.
“We need to consider tailoring vaccine formulations and dosages based on the sex of the vaccine recipient as well as their age,” said researcher Sabra Klein, PhD.
Understanding immune health
To get a better understanding of immune health and to see how young women are outperforming older women and their male counterparts, the researchers conducted two studies: one on humans and the other on mice.
For the first study, participants were divided into two groups based on age: those aged 18-45 and those 65 and older. All participants were given the 2009 H1N1 flu vaccine, after which the researchers analyzed their bodies’ immune response to the injection.
Younger women had the best immune response, as their bodies produced higher levels of the IL-6 protein, which helps the body limit flu-related inflammation and promotes healthy lung function. The younger women in the study also had a better immune response than all men, but the most significant difference was between younger women and older women.
When it came to the mice, the researchers analyzed very similar results, as young, female mice had the best outcomes after receiving the flu vaccine when compared with male mice and older mice. The researchers determined that sex hormones played a large role in how older male and female mice responded to the flu vaccine, with levels of estrogen and testosterone are significantly altered in later years.
Moving forward, the researchers hope that healthcare officials use these findings to alter the way older people receive vaccines, as factors like aging and gender play a role in how the body responds.
“What we show here is that the decline in estrogen that occurs with menopause impacts women’s immunity,” said Klein. “Until now, this hasn’t been considered in the context of a vaccine. These findings suggest that for vaccines, one size doesn’t fit all -- perhaps men should get larger doses, for example.”
The full study has been published in the journal npj Vaccines.