• A shingles vaccine was tied to a 20% drop in new dementia cases over seven years.
• The U.K. rollout created a natural experiment using birthdate eligibility.
• Reduction was especially strong in women, beyond the effects on shingles itself.
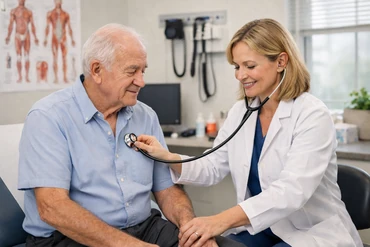
Researchers at Stanford Medicine dove into health records from older adults in Wales to explore the link between the shingles vaccine and the risk of dementia.
They focused on those eligible for the live-attenuated shingles vaccine (Zostavax) based on an exact birthdate cutoff: anyone born on or after September 2, 1933 was eligible, while those born just before weren’t.
Because both groups were nearly identical in age, health, and behavior — except for vaccine eligibility — this setup acted like a “natural randomized trial.”
The result? Receiving the shingles vaccine was associated with a 20% lower chance of developing dementia over the next seven years, even after accounting for who actually got vaccinated.
“All these associational studies suffer from the basic problem that people who get vaccinated have different health behaviors than those who don’t,” researcher Pascal Geldsetzer, M.D., Ph.D., said in a news release. “In general, they’re seen as not being solid enough evidence to make any recommendations on.”
The study
For the study, the researchers used a regression discontinuity design — it allows them to compare people who are alike except for being eligible for vaccination. By looking at those born just before and after the September 1933 cutoff, they ensured both groups were very similar. One group had a 47.2% vaccination rate, while the other had only 0.01%.
Health records were tracked for seven years, noting new dementia diagnoses. To make sure the vaccine itself was the key difference, they checked that the groups didn’t differ in other diseases, doctor visits, or preventive health behavior. They even used alternative analyses to confirm the findings held up no matter how they looked at the data .
The study
The researchers found that there were fewer dementia cases overall. Being eligible for the vaccine cut new dementia diagnoses by 1.3 percentage points, or about 8.5% fewer cases.
In participants who actually got the shot, the reduction jumped to 3.5 points, a 20% drop in dementia risk.
“It was a really striking finding,” Dr. Geldsetzer said in the news release. “This huge protective signal was there, any which way you looked at the data.”
The team also learned that women had greater protective cognitive benefits than men. Though the vaccine lowered dementia risk for both sexes, the effect was significantly stronger in women.
What this means for you
The findings highlight a bonus to getting your shingles vaccine: the potential to protect your brain. Scientists are still trying to figure out why it works — whether it’s because the vaccine stops inflammation-causing shingles outbreaks, or if the vaccine primes the immune system in a way that wards off dementia.
While the study is robust, with careful methods that reduce bias, it’s still observational. That means it can show a strong connection, but not absolute proof. The researchers stress the need for randomized clinical trials before making firm claims.